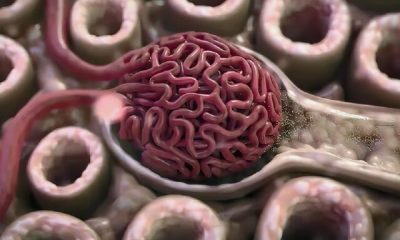
Artificial intelligence identifies cancer killer cells. Using artificial intelligence, scientists have developed a predictive model to identify the most powerful cancer-killing immune cells and deliver cancer immunotherapy.
Artificial intelligence identifies cancer killer cells
A new predictive model can be used in conjunction with multiple algorithms for personalized cancer treatment that matches treatment to the unique cellular makeup of each patient’s tumors.
According to Science Daily, “Alexandre Harari” from the “Ludwig Cancer Research Center”, who supervised this research along with “Rémy Pétremand”, a graduate of this center, said: Artificial intelligence in cell therapy is a new work and may be able to change the treatment method and provide new clinical options to patients.
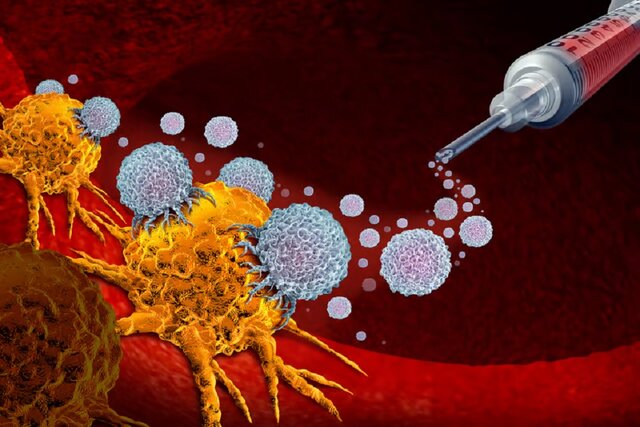
Cellular immunotherapy involves extracting immune cells from a patient’s tumor, engineering them to enhance their natural cancer-fighting abilities, and transplanting them back into the body after they have grown. T cells are one of two main types of white blood cells, or lymphocytes, that circulate in the blood and seek out cells infected with viruses or cancer.
T cells that infiltrate solid tumors are known as tumor-infiltrating lymphocytes (TILs). However, not all tumor-infiltrating lymphocytes are effective in recognizing and attacking tumor cells. Harari explained: Actually, only a part of the lymphocytes react to the tumor and most of them are observers. The challenge we faced was to identify a small number of tumor-infiltrating lymphocytes. These lymphocytes are equipped with T cell receptors that can recognize antigens on the tumor.
To do this, Harari and his team developed an artificial intelligence-based predictive model called TRTpred that can rank T-cell receptors, or TCRs, based on their target tumor reactivity. To develop TRTpred, they used 235 T-cell receptors collected from patients with metastatic melanoma who had previously been classified as tumor-reactive or non-reactive. The research group loaded the gene expression profile of T cells bearing each T cell receptor into a machine learning model to identify patterns that distinguish tumor-reactive T cells from their inactive counterparts.
TRTpred can learn from a T-cell population and create a rule to apply to a new population, Harari explained. So, when faced with a new T-cell receptor, the model can read its profile and predict whether the tumor will respond.
The TRTpred model analyzed tumor-infiltrating lymphocytes in 42 patients with melanoma and gastrointestinal, lung, and breast cancers and identified tumor-reactive T cell receptors with 90% accuracy. The researchers modified their tumor-infiltrating lymphocyte selection process by using a secondary filter that screens only tumor-reactive T cells; That is, only cells that have a strong connection to tumor antigens.
“TRTpred is exclusively predictive of whether or not the T cell receptor is reactive to the tumor, but some tumor-reactive receptors make a strong binding to tumor cells and are therefore very effective,” Harari said. While others do it out of laziness. Distinguishing between strong and weak connections indicates effectiveness.
The researchers showed that T cells identified as tumor reactants by TRTpred and the secondary algorithm are often located in tumors. The findings of this study are in line with other studies that show that effective T cells usually penetrate deep into the tumor.
Next, the researchers introduced a third filter to maximize the detection of tumor antigens. “We want to maximize the chance that tumor-infiltrating lymphocytes will target as many different antigens as possible,” Harari said.
This final filter organizes T cell receptors into several groups based on similar physical and chemical properties. The hypothesis of the researchers is that the T cell receptors in each cluster recognize the same antigen. “So we choose one T-cell receptor in each cluster to amplify to increase the chance of targeting a specific antigen,” said Vincent Zoete, a researcher at the Ludwig Cancer Research Center who developed the T-cell receptor clustering algorithms.
Read more: Discovery of 32 new cancer drugs with the help of artificial intelligence
The researchers call the combination of TRTpred and algorithmic filters “MixTRTpred”.
To validate their method, Harari’s group implanted human tumors into mice, extracted T-cell receptors from their tumor-infiltrating lymphocytes, and used the MixTRTpred system to identify tumor-reactive T cells and multiple antigens in the target tumor. put. Next, they engineered T cells obtained from mice to express T cell receptors and showed that these cells could destroy tumors when transferred to mice.
“George Coukos”, one of the researchers of this project, who is planning to launch the first stage of clinical trial to test this technology in patients, said: This method promises to overcome some of the shortcomings of treatment based on tumor infiltrating lymphocytes. Especially for patients dealing with tumors that are unable to respond to such treatments. Our joint efforts are creating a completely new way of T-cell therapy.
This research was published in “Nature Biotechnology” magazine.



 Technology9 months ago
Technology9 months ago


 Technology10 months ago
Technology10 months ago


 Technology9 months ago
Technology9 months ago


 Technology11 months ago
Technology11 months ago


 AI1 year ago
AI1 year ago

 Humans1 year ago
Humans1 year ago


 Technology10 months ago
Technology10 months ago

 Technology11 months ago
Technology11 months ago